
An 8-year audit of the clinical profile, surgical indications and therapeutic outcomes of total hip arthroplasty in a sub-Saharan Africa setting: a retrospective cohort study
Introduction
Total hip prosthesis is a device implanted in the body to replace the connection between the femoral bone and the pelvic bones (illicit bones) to restore a function that is compromised. On the other hand, total hip arthroplasty (THA) is one of the most successful reconstructive surgeries in orthopedics since 1950s (1). Despite no international consensus position for surgical indications of hip arthroplasty, the main indications of THA are osteoarthritis, osteonecrosis, femoral neck fracture, dysplasia of the hip, and inflammatory arthritis (2). Furthermore, surgical management depends on the clinical state of the patient and radiological findings (1,2).
With more than one million procedures undertaken worldwide, this procedure is commonly practised in the United Kingdom and the United States. In low- and middle-income countries, there is equally a steady rise in the realization of this surgical procedure (3). This study aimed to determine the socio-demographics, clinical characteristics, surgical indications and outcomes of patients treated for THA in an urban setting of Cameroon. We present the following article in accordance with the STROBE reporting checklist (available at https://jxym.amegroups.com/article/view/10.21037/jxym-21-2/rc).
Methods
Study design, setting, and participants
This was a retrospective cohort study entailing the chart review of all consecutive patients with complete medical records of operated for THA over an 8-year period from 1st January 2010 to 31st December 2017. Our study was conducted in the Orthopedic and Traumatology Surgical department of the National Social Insurance Fond Hospital, Yaoundé Cameroon. This hospital serves as a tertiary facility in Yaoundé for the referral of patients from primary and secondary healthcare centers in Yaoundé and its environs. This surgical department is specialized in the management of almost all child and adult surgical pathologies. The Surgical department is run by two orthopedist surgeons, one general practitioner and a team of six nurses. The unit is made up of a 16-bed-ward and has an operating room annexed to it equipped with a C-arm fluoroscopy and diverse surgical orthopedic equipment.
Data collection and sampling
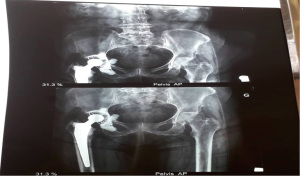
All THA were performed as open surgery (Figure 1) under combined spinal-epidural anesthesia in 63% and general anesthesia in 37% of cases. We performed a chart review of the medical records in the archives of the Orthopedic and Traumatology Surgical department and operating notes of the theatre of the hospital using a pilot pre-tested structured collection sheet for each patient operated for THA. The sampling method was consecutive. The minimal sample size was calculated assuming a 1.3% (4) hospital prevalence rate of THA and a precision of 5% (5), hence a minimum of 32 patients operated for THA as study participants. Variables extract from medical records were socio-demographics characteristics (age and gender), clinical characteristics (symptoms and signs, comorbidities, preoperative hip function assessed using the Postel Merle d’Aubigné (PMA) score and radiological signs, surgical indications, types of prostheses used, and outcomes of treatment.
Diagnostic criteria and outcome
The diagnosis of hip surgical pathologies warranting THA was by frontal and lateral X-rays in first intention and only supplemented by a CT-scan in ambiguous cases. Outcome after surgery was classified based on the functionality of the operated hip as satisfactory recovery (complete regression of pain, normal alignment of both lower limbs), fair recovery (partial regression of pain, incomplete or normal alignment of both lower limbs), limb shortening (a reduction of at least 0.5 cm of the operated limb, neuralgia or nerve damage and persistence of the analgesic).
Statistical analysis
The collected data was analyzed using SPSS version 22. Tables and figures were used to summarize the results. Qualitative variables (gender, clinical characteristics and radiological signs, indications, types of prostheses) were described in terms of numbers and percentage. Quantitative variables (age) were summarized in mean and standard deviation. All data entered were cross-checked trice before entry and analysis to reduce bias. Given that the results were presented in a descriptive form, no statistical test used to reduce bias was used. Variables with too much missing data precluding meaningful analyses and files of patients loss to follow-up were excluded.
Ethical considerations
The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). Ethical clearance was obtained from the Institutional and Ethical Committee of the University of Douala, Cameroon under the number 1,538 CEI-UDO/04/2018/T. Administrative authorization was also granted by the ethics committee of the National Social Insurance Fond Hospital, Yaoundé Cameroon under the number 06/18DCHE/DA/ EC-CHE/NSF. Patients’ medical records were kept confidential by the anonymity of the data collection sheets and individual consent for this retrospective analysis was waived.
Results
General characteristics of the study population
During the period, we found a total of 54 files of patients operated for THA. Fifty files were exploitable (response rate =86.2%). Among the four files excluded, three were incomplete and one had no clear diagnosis. Figure 2 shows a flow chart of files reviewed and studied. The sample consisted of 31 (62%) men and 19 (38%) women with a sex ratio of 1.6 in favor of males. The age of patients who underwent THA ranged from 23 to 94 years with an average age of 54.8±17.1 years.
Clinical characteristics of patients
Comorbidities
Thirty-four patients (68%) had a history of alcohol abuse, seven patients (14%) had history hypertension, and long-term corticosteroid therapy use in 3 (6%) patients. A past history of accidental fall was present in 5 (10%) patients (Table 1).
Table 1
| Variables | Categories | Frequency, n=50 | Percentage (%) |
|---|---|---|---|
| Past history | Alcohol abuse | 34 | 68 |
| Hypertension | 7 | 14 | |
| Accidental fall from their height | 5 | 10 | |
| Prolonged corticosteroid use | 3 | 6 | |
| Diabetes mellitus | 0 | 0 | |
| Sickle cell disease | 0 | 0 | |
| Others | 4 | 8 | |
| Symptoms and signs | Pain | 49 | 98 |
| Functional impotence | 16 | 32 | |
| IM shortening | 31 | 62 | |
| Walking | With crutch | 15 | 30 |
| Lameness with stick or cane | 20 | 40 | |
| Lameness without stick or cane | 11 | 22 | |
| Normal | 4 | 8 | |
| PMA score | NA | 1 | 2 |
| <18 | 48 | 96 | |
| >18 | 1 | 2 | |
| Degree of pain | Mild | 2 | 4 |
| Moderated | 35 | 70 | |
| Severe | 13 | 26 | |
| Localization of pain | Hip | 19 | 38 |
| Hip and thigh | 7 | 14 | |
| Folds of the groin | 23 | 46 | |
| NA | 1 | 2 | |
| Periodicity of pain | During physical activity | 7 | 14 |
| When walking | 32 | 64 | |
| At rest | 11 | 22 | |
| Radiological signs (Crown and Ranawat score) | Grade 1 | 10 | 20 |
| Grade 2 | 2 | 4 | |
| Not avalable | 38 | 76 | |
| Ficat score | Ficat 3 | 7 | 14 |
| Ficat 4 | 18 | 26 | |
| Classification of Garden | Garden 3 | 1 | 2 |
| NA | 9 | 18 | |
| Other signs | Destruction of articular cartilage with | 8 | 16 |
| pinching of the joint space | – | – | |
| Hip prothesis in normal place | 1 | 2 | |
| Dislocated hip prothesis | 2 | 4 | |
| Unveiling hip prothesis | 2 | 4 | |
| Surgical indications | Necrosis of the femoral head | 26 | 52 |
| Coxarthrosis | 16 | 32 | |
| Dysplasia | 12 | 24 | |
| Fracture of the femoral neck | 10 | 20 | |
| Detection of prosthesis | 5 | 10 | |
| Prosthesis dislocation | 2 | 4 | |
| Prosthesis replacement | 2 | 4 |
IM, lower limb; PMA, Postel Merle D’Aubigné; NA, none.
Clinical evaluation
The left side was the most affected in 36 (74%) patients versus eight (16%) patients with right hip disease. In seven patients (14%) the involvement was bilateral. For those with bilateral hip disease, the surgery was performed in two steps never both sides concomitantly. The functionality of the hip was evaluated by the mean PMA score. We had a score of less than 18 in 49 (98%) patients. That is 49 out of 50 patients had a physiologically abnormal hip. We had 16 (30%) patients with functional impotence requiring the use of a pair of crutches, 20 (40%) patients had lameness of the lower limb due to hip disease requiring the use of a walking stick and 11 (22%) cases of lameness without not requiring the use of a walking stick was observed. More than half (62%) of the patients had lower limb shortening, 31 patients (Table 1). In our study population, pain was the major complaint in 98% of cases. In 23 (46%) patients it was localized to the fold of the ipsilateral groin. The moderate degree of pain was predominantly represented in 35 (70%) cases (Table 1). This pain was mechanical in 78% of cases: 64% (32 patients) during walking and 14% (7 patients) during physical activity. Only 22% of cases had inflammatory pain (Table 1).
Radiological signs
Standard radiographs demonstrated hip status, radiological findings, and severity of the lesion as presented in (Table 1). Garden’s classification in femoral neck fractures was noted in only one out of 10 cases and this fracture was classified as Garden III. In our case series, we found records containing cumulative radiological signs. This is explained by the fact that a patient could carry several lesions affecting the same joint at the same time.
Indications of THA
Individuals primary indications
In our series, we found the primary indications in 42 (84%) files. The most represented indications were degenerative hip disorders in 39 (78%) cases of which 24 (48%) of cases had necrosis of the femoral head (NFH) and 2 (3%) of cases had hip osteoarthritis. Dysplastic indications were not an absolute indication because acetabular dysphasia was always associated with a degenerative lesion in 10 cases (20%) or a traumatic lesion 2 (4%) cases. We thus identified 23 files containing unique indications, among which: 13 (26%) with NFH only, 4 (8%) with hip osteoarthritis, 6 (12%) with fracture of the femoral neck and finally no record with dysplasia as a single indication (Table 2).
Table 2
| Indications of THP | Necrosis of the femoral head | Coxarthrosis | Dysplasia | Fracture of the femoral neck | Decement of THP | THP dislocation | THP replacement | Total [%] |
|---|---|---|---|---|---|---|---|---|
| Necrosis of the femoral head | 13 | 3 | 8 | 0 | 0 | 0 | 0 | 24 [48] |
| Coxarthrosis | – | 4 | 2 | 3 | 0 | 1 | 1 | 15 [30] |
| Dysplasia | – | – | 0 | 0 | 0 | 0 | 0 | 10 [20] |
| Fracture of the femoral neck | – | – | – | 6 | 1 | 0 | 0 | 10 [20] |
| Decement of THP | 4 | 0 | 0 | 5 [10] | ||||
| THP dislocation | – | – | – | – | – | 1 | 0 | 2 [4] |
| THP replacement | – | – | – | – | – | – | 1 | 2 [4] |
| 1 indication | 13 | 4 | 0 | 6 | 4 | 1 | 1 | 29 [58] |
| 2 indications | 11 | 10 | 10 | 4 | 1 | 1 | 1 | 19 [38] |
| 3 indications | 2 | 2 | 2 | 0 | 0 | 0 | 0 | 2 [4] |
THP, total hip prosthesis.
Secondary indications
In our series, we identified 8 (16%) cases with secondary indications of hip arthroplasty, the most common of which was 4 (8%) prostheses. Independently, we had 4 (8%) cases of denture disruption, 2 (4%) cases of prosthesis dislocation, and 2 (4%) cases of prosthesis replacement (Table 2).
Associated indications
The basis of our table shows the summary of the total number of indications in each patient: 29 cases (58%) with a single indication, 19 cases (38%) had two indications, and finally, 2 cases (4%) had three indications (Table 2).
Postoperative evaluation
Functional recovery
In our series, 45 cases (90%) noted satisfactory progression with complete regression of pain, normal alignment of both lower limbs after 5 years of clinical and radiological follow-up (Figure 3). Five (10%) cases had a fair outcome: 3 cases with shortening of 0.5 cm of the operated limb; 1 case with the persistence of the analgesic position; 1 case with nerve damage.
Brief description of surgical procedure the different prostheses in the study population (Table 3)
Table 3
| Variables | Categories | Frequency (n=50) | Percentage (%) |
|---|---|---|---|
| Type of prosthesis | Moore | 0 | 0 |
| Bipolar | 0 | 0 | |
| THP | 50 | 100 | |
| Prosthetic head diameter | 28 cm | 50 | 100 |
| Prosthetic cone diameter | 12/14 cm | 50 | 100 |
| Shape of the stem | Anatomic | 50 | 100 |
| Stem size | 10 | 8 | 16 |
| 12 | 7 | 14 | |
| 7 | 8 | 16 | |
| >12 | 27 | 54 | |
| Mode of fixation | Cemented | 50 | 100 |
THP, total hip prosthesis.
In 50 (100%) of cases, the prosthesis used was the total hip prosthesis type. The outer diameter of the cup went from 44 to 56 mm with an average of 50 mm. Regarding the caliber of the prosthetic head, 48 (92% of the cases had a diameter of 22.2 mm, 8% diameter of 28 mm and the diameter 32 mm was never used. All the prostheses were cemented and the installation of the cement was manual. All the THA put in place had a metal/polyethylene friction torque. The route the most used abroad was the anterolateral approach (Watson jones).
Discussion
In this retrospective cohort study carried we aimed to determine the socio-demographic characteristics, clinical presentation, etiologies, surgical indications and outcomes of THA in the first ever longest review period of 8 years in Africa. The goal being to equally assess the feasibility and safety of this complex and relatively expensive orthopedic surgical procedure in a low-resource country of Africa, currently witnessing an improvement in global surgery. We found that the mean age of patients was 54.8±17.1 years and 62% were males. The most common indications for THA were degenerative hip disorders (78%). The most affected hip was the left (72%). The main comorbidity found were chronic alcohol abuse (68%). Overall, 38% and 4% of patients had two and three surgical indications for THA respectively. Globally, good functional recovery or treatment outcomes were satisfactory in over 90% of patients operated for THA at 5 years of clinical and radiological follow-up.
Age is an important epidemiological element in the use of a hip prosthesis because it determines the functional outcome and the longevity of the prosthesis (4). The outcomes of hip prostheses before the age of 50 are traditionally worse than those of older populations (5). The risk of death in these young people is 1.8-fold increase for Eng (4). In our series, the average age of patients who received a hip replacement was 54.8±17.1 years. The extremes were 23 and 94 years old. The relatively advanced age of our study population could be explained by the fact that in our context, relatively elder adults are more prone to these risk factors (Table 1). Our results corroborate with those of Magoumou et al. (3) who found a mean age of 69 years with a tendency for adults aged below 65 years at increased risk of THA. Our results are higher to those of Hwang et al. (6) in South Korea, Faldini et al. (7) in Bologna (Italy) and Magoumou et al. (3) in Kazablanka (Morocco) due to limiting the age of the study population. In contemporary literature, there is a female preponderance among THA patients (2), due to degenerative hip disorders like osteoporosis with resultant pathological hip fractures which occur after menopause. After accidental falls. Magoumou et al. (3) found a similar female predominance of 60.47%, with a sex ratio equal to 0.65. Unlike observations made by Hwang et al. (6) and Migaud et al. (8), we found a male preponderance of 62% with a gender ratio of 1.6, probably explained by the fact that in our Cameroonian context alcohol abuse is more common among men than females and this may lead to higher rates of accidental falls in males requiring THA.
In contrast to our findings, Magoumou et al., observed a predominance of right hip pathologies requiring THA (55.81%) against 34.88% on the left and 9.3% bilaterally (3). Hence, we can deduce that the damage to the side is independent of the lesion and can occur randomly. When the hip is affected by a pathological procedure, the clinical expression is generally based on three functional signs associated with various degrees: pain, loss of mobility and lameness. These signs lead to patient discomfort. Although not alone, it is a pathology responsible for certain discomforts in the young subject. The indication of a hip prosthesis in young adults in our series was NFH in 52% of cases for an age group of 36–50 years. Unlike Magoumou et al. (3) for whom hip osteoarthritis is the priority indication. Our results are explained by the fact that young populations are prone to vascular microlesions of the femoral head in the course of their various activities (exercise named the giraffe head in military training). According to the current literature, corticosteroids constitute a major risk factor in THA patients, followed by chronic alcoholism (9). In our series, alcohol abuse was observed in 68% of cases; and long-term corticosteroids use in 6% of cases. However, our findings does not necessarily imply that corticosteroids are used little in our context, but rather we do not have good traceability of their use because of the illegal manipulations (prescription by sellers of drugs). Our results concur with those of Magoumou et al. (3) and Migaud et al. (8).
At the inspection, lameness remains the most marked sign and it signifies the pain of the hip joint and the inability of the gluteal muscles to compensate for this joint failure. The mobilization for it must be passive but especially active and comprises various maneuvers (flexion, extension, internal rotation, and external rotation, and also abduction and adduction); any limitation or pain caused by any of these maneuvers leads to hip involvement (10). Contrary to our series, hip pain was the most common presenting complaint (98%), of mechanical type in more than half of the patients, with lameness when walking in 60% of cases. On clinical examination, shortening of the lower limb is found. The limitation of the passive and active movements was represented in our files by the MAP score always lower than 18 in all our patients. The radiographic assessment includes hip shots seen from the front and in profile. The radiological modifications have been the subject of various classifications, of which that of Arlet and Ficat remains the most used. In this classification, the radiographic aspects are grouped into 4 stages (11). In our series, stage 4 was represented in 18 (26%) of 26 patients (52%) with NFH, followed by stage III with 8 (16%) patients.
Hip osteoarthritis is a common condition occupying the 1st place in the pathology of the hip according to the review of the literature, this being due to the aging of the population among the Westerners. According to our study, it occupies the second place in 32% of patients with an age between 50–65 years. Our results are similar to those of Yuasa et al. (12), in whom the mean age of hip osteoarthritis patients was 73 years for 50–80 years. This could be due to the absence or delay in the diagnosis and treatment of certain inflammatory conditions affecting the hip in the Cameroonian context. According to Vingård et al. (13), hip osteoarthritis increases with age because of obesity, an established risk factor for THA. The hip prosthesis on hip dysplasia remains a challenge for the surgeon. Proper planning and surgical techniques are essential to ensure a better outcome (3). In our study, dysplasia was associated with a degenerative lesion: in 16% with avascular Necrosis (AVN) and 4% with hip osteoarthritis. In Western literature, there is a female predominance among hip replacement patients. This is re-iterated by Chougle et al. (14) who found 98% of women with THA compared to 2% of men for a sample of 42 patients. These results are similar to those of Mu et al. (15) (China). According to the radiological evaluation, patients had Crowse Stage IV dysplasia (6) concurring with findings of Mu et al. (15) in China and Sofu et al. (11) in Turkey. In our series, stage I and II were the most common. This could be explained by the frequency of child carriage (corrective factor) on the back in our context. Our results appear to be similar to those of von Kries et al. (16) who showed that dysplasia in Germany and Austria is no longer an indication for hip arthroplasty. This is because in these countries the pelvic ultrasound is a routine examination between 4 and 6 weeks postpartum, systematically detect these malformations and treat them either orthopedically or surgically (16).
In our case series, one of the major risk factor for hip fractures was accidental falls. This drop could be explained by the fact that older people are prone to decreased hearing, vision and balance. In our series, we had 8 hip prostheses: 4 prosthetic incisions; 2 dislocations of prostheses and 2 prosthesis replacement (in patients with THA for more than 10 years). Of all these occasions, 4 THA were previously made at the National social Insurance Fond Hospital, 2 in Europe and the rest without precision. We can explain the occurrence of these indications in our context by the non-respect of the postoperative rules (avoidance of sudden movements, dwelling in the hilly access neighborhoods, precarious lifestyle, indigenous toilets and poor personal hygiene, without forgetting the surgical techniques sometimes inappropriate, inappropriate material). According to Ficat (10) several factors were considered to be determinants in the revision of total hip prostheses, such as: age, the presence of a “hard-soft” type of friction. The prosthesis most used in our context was the 100% total hip prosthesis because it is the only one easily accessible and indicated. The traditional ceramic-ceramic friction torque is the reference, and it has a longer clinical decline (14). Survival is 85% at 20 years, 80% at 25 years and 78% at 30 years (16). Polyethylene remains the most widely used material because of its low cost and ease of manufacture (14). In our study, the polyethylene-metal pair is used at 100% more than 10 years. This is explained by the fact that it releases very little particles from friction and releases very little energy during movement, therefore a good tolerance of patients. The survival of uncemented THA is inferior to that of cemented THA; this could be due to the poor performance of uncemented THA. Kaplan-Meler in his study, found: 94% of patients with cemented THA and whose lifespan of the prosthesis is 10 years (16). In our series, the most used fixation method was the cemented THA in all our patients because after several tests, the performance of the cemented THA extended for a minimum of 5 years despite the hard activities we face.
Magoumou et al. (3) in their study found a good radiological evolution in 89.6% of patients; a good clinical course in 17% of patients; and 23.4% of patients lost to follow-up in a series of 40 cases treated with a hip prosthesis. Similar findings have been described by several authors following open reduction and internal fixation of fractures in sub-Saharan Africa (17-19). They scored well with an average PMA score of 16.7. In our series, 45 cases (90%) noted satisfactory progression with complete regression of pain, normal alignment of both lower limbs. 5 cases had a fair evolution: 3 cases with shortening of the operated limb of 0.5 cm. In our series, complications were assessed via the telephone. For valid numbers and patients who picked up their phone, we were able to gather on the 5 cases the following information: 3 cases with a shortening of the operated limb of 0.5 cm for information because the difference in length is a postoperative complication when it is equal to 3 cm and more; 1 case with the persistence of the analgesic position; 1 case with nerve damage.
The limitations of the current study are the lack of well-illustrated information in the files, namely: the radiographic reports, the functional evolution; poor tenuous records marked by incomplete writing of medical observations and number of patients’ phones not available for most. However, using a robust study design, our study is one of the first to illustrate the feasibility and safety of THA (previously thought to be impossible to perform in low-resource settings due to the complexity of the surgical technique, the lack of the required surgical infrastructure and the relatively high financial cost of the surgery) in an era of advanced global surgery. Our findings can be generalized to African settings with the same surgical infrastructure as us especially where a C-arm fluoroscopy is available.
Conclusions
The prosthetic replacement of the hip joint over the last 8 years in this developing country has involved a relatively elderly population with an average age around 55 years and a male predominance. The indications were mostly degenerative followed by traumatic lesions. Globally, good functional scores with satisfactory treatment outcomes were obtained in over 95% of patients operated. However, the majority of degenerative indications must attract the attention of orthopedic surgeons to an early and better management of hip arthropaties.
Acknowledgments
To the medical and nursing staff of the Orthopedic and Trauma Surgery Unit at National social Insurance Fond hospital, Yaoundé Cameroon for the care of the patient. To the AO Alliance who made this study possible.
Funding: None.
Footnote
Reporting Checklist: The authors have completed the STROBE reporting checklist. Available at https://jxym.amegroups.com/article/view/10.21037/jxym-21-2/rc
Data Sharing Statement: Available at https://jxym.amegroups.com/article/view/10.21037/jxym-21-2/dss
Peer Review File: Available at https://jxym.amegroups.com/article/view/10.21037/jxym-21-2/prf
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at https://jxym.amegroups.com/article/view/10.21037/jxym-21-2/coif). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. The study was conducted in accordance with the Declaration of Helsinki (as revised in 2013). Ethical clearance was obtained from the Institutional and Ethical Committee of the University of Douala, Cameroon under the number 1538 CEI-UDO/04/2018/T. Administrative authorization was also granted by the ethics committee of the National Social Insurance Fond Hospital, Yaoundé Cameroon under the number 06/18DCHE/DA/ EC-CHE/NSF. Patients’ medical records were kept confidential by the anonymity of the data collection sheets and individual consent for this retrospective analysis was waived.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Khanduja V. Total hip arthroplasty in 2017—current concepts and recent advances. Indian J Orthop 2017;51:357-8. [Crossref] [PubMed]
- Pivec R, Johnson AJ, Mears SC, et al. Hip arthroplasty. Lancet 2012;380:1768-77. [Crossref] [PubMed]
- Magoumou A, Dabiré N, Andaloussi YE, et al. Total hip replacement in young adults less than fifty year old: our experience. Open J Emerg Med 2008;5:43-74. [Crossref]
- Eng J. Sample size estimation: how many individuals should be studied? Radiology 2003;227:309-13. [Crossref] [PubMed]
- Aldinger PR, Jung AW, Pritsch M, et al. Uncemented grit-blasted straight tapered titanium stems in patients younger than fifty-five years of age. Fifteen to twenty-year results. J Bone Joint Surg Am 2009;91:1432-9. [Crossref] [PubMed]
- Hwang KT, Kim YH, Kim YS, et al. Cementless total hip arthroplasty with a metal-on-metal bearing in patients younger than 50 years. J Arthroplasty 2011;26:1481-7. [Crossref] [PubMed]
- Faldini C, Miscione MT, Chehrassan M, et al. Congenital hip dysplasia treated by total hip arthroplasty using cementless tapered stem in patients younger than 50 years old: results after 12-years follow-up. J Orthop Traumatol 2011;12:213-8. [Crossref] [PubMed]
- Migaud H, Putman S, Krantz N, et al. Cementless metal-on-metal versus ceramic-on-polyethylene hip arthroplasty in patients less than fifty years of age: a comparative study with twelve to fourteen-year follow-up. J Bone Joint Surg Am 2011;93:137-42. [Crossref] [PubMed]
- Kittle H, Ormseth A, Patetta MJ, et al. Chronic corticosteroid use as a risk factor for perioperative complications in patients undergoing total joint arthroplasty. JAAOS Glob Res Rev. 2020;4: e20.00001. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7366416/.
- Ficat P. Traitement chirurgical de la coxarthrose Rev Prat 1974;24:4314-39. [Surgical treatment of coxarthrosis]. [PubMed]
- Sofu H, Kockara N, Gursu S, et al. Transverse subtrochanteric shortening osteotomy during cementless total hip arthroplasty in Crowe type-iii or iv developmental dysplasia. J Arthroplasty 2015;30:1019-23. [Crossref] [PubMed]
- Yuasa T, Maezawa K, Nozawa M, et al. Midterm outcome of total hip arthroplasty for rapidly destructive coxarthrosis. J Orthop Surg (Hong Kong) 2016;24:27-30. [Crossref] [PubMed]
- Vingård E. Overweight predisposes to coxarthrosis. Body-mass index studied in 239 males with hip arthroplasty. Acta Orthop Scand 1991;62:106-9. [Crossref] [PubMed]
- Chougle A, Hemmady MV, Hodgkinson JP. Severity of hip dysplasia and loosening of the socket in cemented total hip replacement. A long-term follow-up. J Bone Joint Surg Br 2005;87:16-20. [Crossref] [PubMed]
- Mu W, Yang D, Xu B, et al. Midterm outcome of cementless total hip arthroplasty in Crowe IV-hartofilakidis type III developmental dysplasia of the hip. J Arthroplasty 2016;31:668-75. [Crossref] [PubMed]
- von Kries R, Ihme N, Altenhofen L, et al. General ultrasound screening reduces the rate of first operative procedures for developmental dysplasia of the hip: a case-control study. J Pediatr 2012;160:271-5. [Crossref] [PubMed]
- Tochie JN, Guifo ML, Yamben MN, et al. A prospective cohort study of the therapeutic patterns, challenges and outcomes of paediatric femoral fractures in a cameroonian tertiary center. Open Orthop J 2017;11:29-36. [Crossref] [PubMed]
- Guifo ML, Tochie JN, Oumarou BN, et al. Paediatric fractures in a sub-saharan tertiary care center: a cohort analysis of demographic characteristics, clinical presentation, therapeutic patterns and outcomes. Pan Afr Med J 2017;27:46. [Crossref] [PubMed]
- Mbonda A, Tchuenkam WL, Tochie JN, et al. Diagnostic and therapeutic challenges of a slipped capital femoral epiphysis in a low and middle income country: a case report and literature review. Open Orthop J 2019;13:152-8. [Crossref]
Cite this article as: Essomba R, Mondji S, Mbonda AN, Tochie JN, Abogo S, Lekina F, Nonga BN. An 8-year audit of the clinical profile, surgical indications and therapeutic outcomes of total hip arthroplasty in a sub-Saharan Africa setting: a retrospective cohort study. J Xiangya Med 2022;7:6.




