Cardio-oncology program: a much needed collaboration in the Middle East
Cancer remains the second leading cause of death in the Western world (1,2), with increasing numbers in the Middle East. Over the last decade, there have been new chemotherapeutic agents such as monoclonal antibodies that target human epidermal growth factor receptor tyrosine kinase inhibitor (TKI) and new generation of anthracyclines that are showing promising results (3,4). However, these agents carry potential cardiotoxic effect (type I and type II) that may result in heart failure (5-7).
While ejection fraction on echocardiography has been the most commonly known parameter to oncologists to assess left ventricular systolic function, it often fails to detect subclinical cardiomyopathy and has several limitations. Indeed, updates in cardiovascular imaging using speckle tracking and strain analysis, have allowed the subclinical detection of systolic dysfunction as evidenced by a decrease in global longitudinal strain (GLS) before a visual drop in ejection fraction is seen (8,9). Recently, an expert consensus was released and adopted by the American Society of Echocardiography and European Association of Cardiovascular Imaging to shed more light on the advantages of using GLS, identifying high risk patients, and setting some guidelines and practical workflow of a collaboration between oncologists and cardiologists (10).
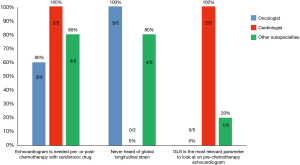
As a non-invasive cardiologist that worked previously in a tertiary cardiac center with established cardio-oncology program in the United States, I moved back to the Middle East to work in private practice where there were no formal cardiooncology programs. However, I was curious to see whether the practicing oncologists are aware and taking advantages of the advancements in cardiac imaging, whether there are remaining gaps and therefore potential room for improvement. To that effect, and during a routine tumor board meeting held in February 2016, I conducted a very brief survey to several oncologists (n=5) that practiced in different private satellite hospitals, cardiologists that are specialists in cardiovascular imaging (n=2), and other internal medicine subspecialists (n=5). The survey asked three simple questions: (I) do you perform/recommend routine echocardiograms pre and/or post chemotherapy cycles for patients receiving anthracycline or TKI chemotherapy agents? (II) have you heard of GLS with echocardiography? (III) which echocardiography parameter you rely mostly on to decide whether to clear a patient for potentially cardiotoxic chemotherapy?
Although the majority of physicians recommended performing echocardiograms, none of the five oncologists knew what GLS was, and none of them obviously chose GLS as an add-on or isolated most important parameter of the echocardiography report (Figure 1).
This survey by no means however, undermines these oncologists who are outstanding physicians saving lives and treating patients at different private hospitals and clinics. It is important to recognize that many of the satellite clinics where these physicians are practicing do not have cardiologists who routinely perform advanced cardiac imaging or report GLS, therefore minimizing their exposure to it. Also, private practice is quite different from the academic setting.
While the survey is obviously limited by the small sample size, it does shed light on the fact that there are significant gaps and much needed work in the field of cardiooncology. Important steps include: (I) educating oncologists about the importance of recognizing subclinical cardiomyopathy and the cardiotoxic effect of the chemotherapy; (II) providing them with the tools and recent advances in imaging to make the diagnosis and reverse the process with the use of cardioprotective medications; (III) launch formal cardiooncology programs and collaboration between oncologists and cardiologists; (IV) have cardiologists attend tumor board meeting and get consulted on clinical cases with high risk patients routinely; (V) organize a cardiooncology session during the oncology scientific meetings (nationally and internationally) to increase awareness and encourage such collaboration that will ultimately result in improved patient care and better outcomes. After all, what would be the benefit of achieving full remission at the expense of ending up with irreversible cardiomyoathy that could have been prevented?
To this effect, multinational efforts have been put to place to initiate cardio-oncology programs while highlighting challenges and solution (11). Indeed, many tertiary hospitals in the United States do not have a dedicated cardiooncology program. Similar challenges exist in the United Kingdom (12), and in Italy (13,14) . While the magnitude of the problem is a major challenge, the equivocal reliability of strain imaging with lack of standardization is another limitation to be surmounted (15).
A recent survey conducted by the American College of Cardiology showed that only 27% of surveyed centers had a dedicated cardiooncology program, and that many did not feel comfortable taking care of cardiovascular complications in cancer patients (16).
The establishment of cardiooncology programs with proper funding and backing up from societies is needed to provide optimal care to cancer patients.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: The author has completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/jxym.2016.12.10). The author has no conflicts of interest to declare.
Ethical Statement: The author is accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Hoyert DL, Xu J. Deaths: Preliminary data for 2011. National vital statistics reports: from the Centers for Disease Control and Prevention, National Center for Health Statistics, National Vital Statistics System. 2012;61:1-51. Available online: http://www.cdc.gov/nchs/data/nvsr/nvsr61/nvsr61_06.pdf
- Santulli G. Epidemiology of cardiovascular disease in the 21st century: Updated numbers and updated facts. Journal of Cardiovascular Disease 2013;1:2326-3121.
- Hojjat-Farsangi M. Small-molecule inhibitors of the receptor tyrosine kinases: promising tools for targeted cancer therapies. Int J Mol Sci 2014;15:13768-801. [Crossref] [PubMed]
- Conte P, Guarneri V. The next generation of biologic agents: therapeutic role in relation to existing therapies in metastatic breast cancer. Clin Breast Cancer 2012;12:157-66. [Crossref] [PubMed]
- Mordente A, Meucci E, Silvestrini A, et al. New developments in anthracycline-induced cardiotoxicity. Curr Med Chem 2009;16:1656-72. [Crossref] [PubMed]
- Ewer SM, Ewer MS. Cardiotoxicity profile of trastuzumab. Drug Saf 2008;31:459-67. [Crossref] [PubMed]
- Perez EA. Cardiac toxicity of ErbB2-targeted therapies: what do we know? Clin Breast Cancer 2008;8:S114-20. [Crossref] [PubMed]
- Thavendiranathan P, Poulin F, Lim KD, et al. Use of myocardial strain imaging by echocardiography for the early detection of cardiotoxicity in patients during and after cancer chemotherapy: a systematic review. J Am Coll Cardiol 2014;63:2751-68. [Crossref] [PubMed]
- Negishi K, Negishi T, Haluska BA, et al. Use of speckle strain to assess left ventricular responses to cardiotoxic chemotherapy and cardioprotection. Eur Heart J Cardiovasc Imaging 2014;15:324-31. [Crossref] [PubMed]
- Plana JC, Galderisi M, Barac A, et al. Expert consensus for multimodality imaging evaluation of adult patients during and after cancer therapy: a report from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging 2014;15:1063-93. [Crossref] [PubMed]
- Okwuosa TM, Barac A. Burgeoning Cardio-Oncology Programs: Challenges and Opportunities for Early Career Cardiologists/Faculty Directors. J Am Coll Cardiol 2015;66:1193-7. [Crossref] [PubMed]
- Cubbon RM, Lyon AR. Cardio-oncology: Concepts and practice. Indian Heart J 2016;68:S77-85. [Crossref] [PubMed]
- Canale ML, Camerini A, Magnacca M, et al. A cardio-oncology experience in Italy: results of a Tuscany regional-based survey. J Cardiovasc Med (Hagerstown) 2014;15:135-40. [Crossref] [PubMed]
- Patanè S. Insights into cardio-oncology: the patient's heavy cancer journey among doubts, controversies and pitfalls. The role of the cardiologist. Int J Cardiol 2015;178:175-7. [Crossref] [PubMed]
- Collier P, Koneru S, Tamarappoo B, et al. Strain imaging to detect cancer therapeutics-related cardiac dysfunction: are we there yet? Future Cardiol 2015;11:401-5. [Crossref] [PubMed]
- Barac A, Murtagh G, Carver JR, et al. Cardiovascular Health of Patients With Cancer and Cancer Survivors: A Roadmap to the Next Level. J Am Coll Cardiol 2015;65:2739-46. [Crossref] [PubMed]
Cite this article as: AlJaroudi W. Cardio-oncology program: a much needed collaboration in the Middle East. J Xiangya Med 2016;1:10.